The Telfer School of Management is the proud presenting sponsor of a series of four webcasts powered by The Globe and Mail Events. Each webcast will highlight one of the four pillars in the Telfer Vision for a Better Canada — a greener, healthier, happier, wealthier and more prosperous Canada for all — through an interview with a Telfer professor, followed by a discussion with a panel of experts.

Even before the pandemic, long wait times, uneven access and mounting costs were common issues in Canadian health care. These challenges have only increased, with health care providers facing a significant backlog in elective surgeries, treatments and tests. How can Canada’s healthcare system recover from the current crisis and move toward a better model?
On November 15, the Globe and Mail hosted a webcast to discuss how health care in Canada should evolve to become more accessible, effective and resilient. One expert looking into these questions is Telfer professor Lysanne Lessard, co-lead of the school’s Learning Health Systems Modeling Lab. In the interview portion of the November event, led by André Picard, health reporter and columnist for the Globe and Mail, Lessard explained how Canada has a unique healthcare system with its own issues. Instead of looking to other countries and importing a model that may not work here, it’s important to focus on what’s being done well in Canada and scale up those successes.
Importance of data collection
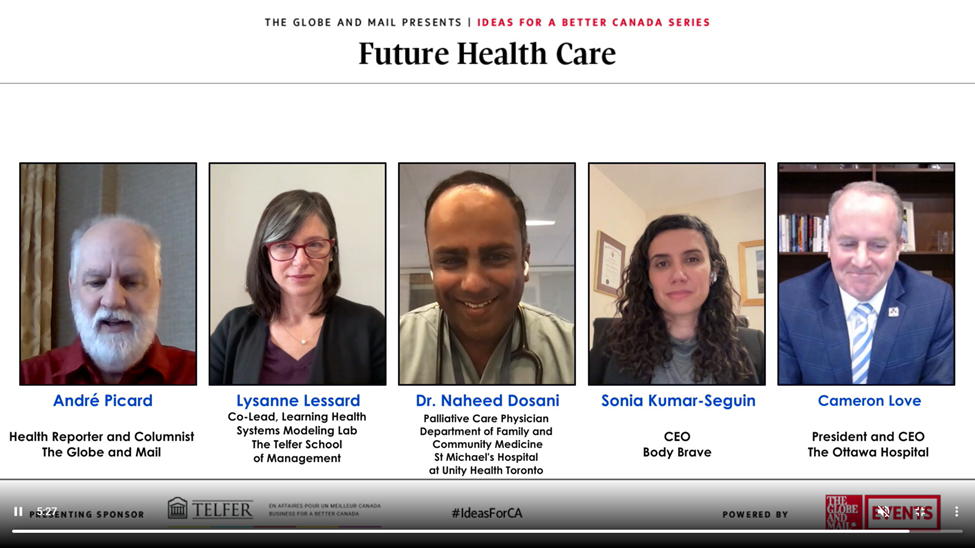
According to Lessard, the healthcare system is complex and difficult to understand. By gathering data on all parts of the patient journey, including interactions with health care providers, experiences with different treatments and overall health outcomes, researchers can gain a more complete picture of the system.
The panelists suggested using technology and data to provide personalized care, for example, using electronic health records to track patient health trends and implementing telemedicine to connect patients with remote providers. This would not only improve patient outcomes, but also reduce costs by preventing chronic conditions from developing, through early detection.
Currently, data on Canadian health care is fragmented and not always accessible. Lessard advocates for a more coordinated and standardized approach to data collection and analysis.
Increased access to primary care

One of the key themes that emerged from the event was the need for increased access to primary care. Today, many Canadians face long wait times to see a primary care provider and often turn to emergency rooms for non-urgent care. This not only puts a strain on the emergency room system, but also leads to fragmented care and potential health risks for patients. The panelists suggested expanding the scope of practice for other health care professionals, such as nurse practitioners and pharmacists.
According to Cameron Love, president and CEO of the Ottawa Hospital, the current system is heavily reliant on hospitals, which are often overwhelmed by patients. This puts a great deal of pressure on hospital staff, who are already stretched thin due to staffing shortages. Love suggested implementing an integrated, comprehensive primary care approach, where patients are assigned a team of health care providers including a doctor, nurse and other health professionals. This would ensure that patients have access to timely, better care.
To learn more about the different approaches to health care, read the article: Canadian health systems need to implement change faster
Personalized preventive care

Another key issue discussed was the need for more personalized and preventive care. The healthcare system is primarily reactive, often treating patients only after they’ve developed a health issue. By shifting the system toward a proactive approach with preventive care, patients could receive targeted support and avoid chronic conditions.
Dr. Naheed Dosani, a palliative care physician at St. Michael’s Hospital at Unity Health Toronto, took part in the panel, alongside Love and Sonia Kumar-Seguin, president and CEO of Body Brave. Dosani discussed the importance of addressing social determinants of health, such as housing and income, to improve overall health outcomes. He said that the healthcare system must work closely with other sectors, such as education and housing.
Dosani also said that palliative care should be a priority in both home and community settings, providing relief from the symptoms, pain and stress of serious illnesses and improving quality of life for both patients and their loved ones.
Reimagining the future of health care
This virtual event provided a thought-provoking discussion about the future of health care in Canada and the ways in which the system could improve. By focusing on greater access to primary care, collaboration and coordination, and addressing social determinants of health, the healthcare system can evolve and provide the high-quality care that Canadians deserve.